Gastroesophageal reflux disease (GERD) is more than just occasional heartburn. In some cases, it can trigger shortness of breath, chest tightness, persistent coughing, and wheezing, leaving sufferers feeling anxious and uncomfortable. Symptoms often worsen after heavy meals, lying down, or consuming spicy and acidic foods, making everyday activities a challenge. While mild episodes may pass quickly, persistent or severe breathing difficulties could signal serious complications that require urgent attention. Understanding these warning signs, common triggers, and how reflux impacts the lungs and airways is essential for managing GERD effectively and protecting your respiratory health.
For severe or worsening symptoms, seeking prompt care at an ER in Pearland can help rule out serious complications and ensure timely treatment.
What Is GERD?
GERD occurs when the lower esophageal sphincter, a muscular valve that normally keeps stomach acid from rising into the esophagus, becomes weak or relaxes inappropriately. This allows acidic contents to move upward, irritating the esophagus lining. Occasional acid reflux is common, but chronic reflux is classified as GERD and can lead to long-term complications if untreated. Symptoms vary in severity, and some individuals may experience frequent discomfort, affecting daily activities and sleep. Recognizing the signs of GERD early can help prevent more serious problems.
Symptoms of GERDThat May Affect Breathing
- Shortness of breath: Some individuals with GERD may experience difficulty breathing, particularly after meals or when lying down. This can feel like a tightness in the chest or a sense of not getting enough air, even without underlying lung disease.
- Chest tightness or pressure: Acid reflux can irritate nerves near the esophagus, causing a sensation of heaviness or pressure in the chest. This symptom is often mistaken for heart-related issues and can increase anxiety if not recognized as reflux-related.
- Persistent cough: Chronic coughing, especially at night or early in the morning, is common in GERD patients. The cough is typically dry and may worsen when lying down or after eating trigger foods, due to irritation of the throat and airway.
- Wheezing: GERD can aggravate asthma or cause asthma-like symptoms, resulting in wheezing or noisy breathing. Airway inflammation from acid irritation can narrow the bronchial passages, making it harder to breathe deeply.
- Throat irritation or hoarseness: Frequent exposure to stomach acid can inflame the throat, causing a scratchy feeling, hoarseness, or a constant need to clear the throat. This is particularly noticeable in the morning or after reflux episodes.
- Difficulty taking deep breaths: Some patients may feel as if they cannot fully expand their lungs, especially after acid reflux episodes. This symptom is usually temporary, but it can become more noticeable with chronic GERD.
- Feeling of a lump in the throat (globus sensation): Acid irritation or inflammation of the esophagus may create a sensation of a lump or tightness in the throat. This can make swallowing uncomfortable and may be accompanied by mild choking or gagging sensations.
If symptoms suddenly worsen or become severe, finding an ER near me is important for immediate evaluation and care.
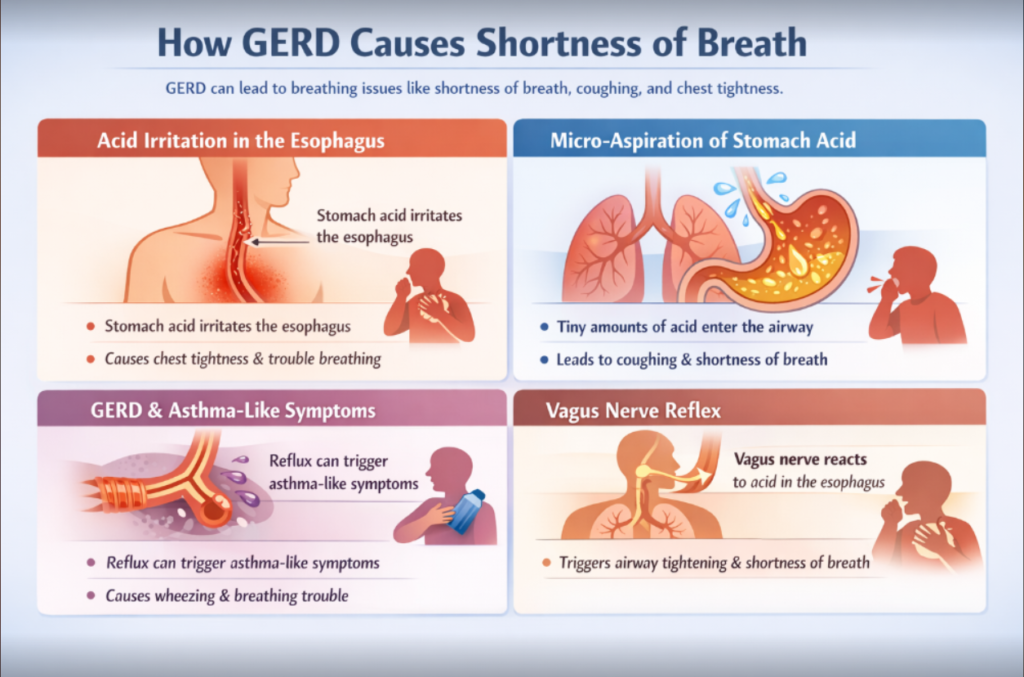
How GERD Causes Shortness of Breath
GERD can affect breathing through several mechanisms, causing shortness of breath, coughing, and chest tightness. Understanding these processes helps explain why some people feel respiratory symptoms even without direct lung disease.
Acid Irritation in the Esophagus
When stomach acid irritates the esophagus, it can stimulate nerves that influence breathing. This irritation may trigger a sensation of chest tightness or difficulty taking deep breaths. Frequent exposure can increase esophageal sensitivity, making the airways react more strongly over time. Acid irritation is one of the most common ways GERD can impact respiratory function, especially during or after reflux episodes.
Micro-Aspiration of Stomach Acid
Occasionally, tiny amounts of stomach acid can enter the airway, a process called micro-aspiration. This can inflame the lungs or throat, leading to persistent coughing, wheezing, or difficulty breathing. Symptoms often worsen at night or after meals when acid is more likely to move upward. Repeated micro-aspiration over time may increase the risk of chronic respiratory issues or worsen preexisting conditions.
GERD and Asthma-Like Symptoms
Acid reflux can exacerbate asthma or cause asthma-like symptoms by irritating the airways. Inflammation and narrowing of the bronchial passages may occur, resulting in coughing, wheezing, or shortness of breath. Patients with preexisting asthma often notice flare-ups following reflux episodes. Recognizing the connection between GERD and respiratory symptoms can help individuals manage both conditions more effectively.
Vagus Nerve Reflex
The vagus nerve connects the esophagus and lungs, allowing acid irritation to trigger reflexive airway responses. When the nerve senses acid in the esophagus, it can cause sudden tightening of the airways or difficulty breathing. Even without direct aspiration, this nerve reflex can produce noticeable respiratory symptoms. This mechanism explains why some patients feel short of breath during reflux episodes, particularly after eating or when lying down.
Risk Factors That Can Worsen GERD
Several lifestyle habits and health conditions can increase GERD symptoms and affect breathing:
- Obesity: Extra abdominal pressure pushes stomach acid upward, increasing reflux episodes.
- Large or late-night meals: Heavy meals close to bedtime make acid flow back more easily, especially when lying down.
- Spicy, fatty, or acidic foods: These can irritate the esophagus or relax the lower esophageal sphincter, triggering reflux.
- Smoking: Weakens the esophageal sphincter and reduces saliva, which normally neutralizes stomach acid.
- Alcohol consumption: Relaxes the esophageal sphincter and can irritate the esophagus lining.
- Pregnancy: Hormonal changes and pressure from the growing uterus can worsen reflux symptoms.
- Hiatal hernia: Part of the stomach pushes through the diaphragm, making reflux more likely.
- Certain medications: Some asthma, blood pressure, and pain medications may increase acid backflow or irritate the esophagus.
Being aware of these factors helps in taking preventive steps and reducing the severity of symptoms.
When GERD Is Dangerous
Most cases of GERD are manageable, but untreated reflux can cause serious complications. Chronic acid exposure can damage the esophagus, leading to painful ulcers, bleeding, or scarring. In severe cases, Barrett’s esophagus, a precancerous condition, may develop, increasing the risk of esophageal cancer. Persistent reflux can silently progress, causing long-term digestive problems if ignored.
GERD can also affect the lungs and heart. Severe shortness of breath, chest pain, or worsening cough may indicate airway irritation or cardiac strain. Difficulty swallowing, choking, or unexplained fatigue should never be ignored. For children showing severe symptoms, visiting an emergency room for pediatrics ensures specialized care and timely intervention. Prompt medical evaluation is essential to prevent permanent damage or life-threatening complications.
Medications & Treatment Options
Managing GERD effectively can help reduce both digestive discomfort and breathing-related symptoms like shortness of breath or coughing.
Lifestyle Changes
Adjusting daily habits can significantly reduce reflux episodes. Eating smaller meals and avoiding known trigger foods, such as spicy or fatty dishes, helps prevent acid reflux. Remaining upright for several hours after eating minimizes nighttime symptoms. Elevating the head while sleeping can also reduce reflux severity. Maintaining a healthy weight supports long-term relief and decreases abdominal pressure on the stomach.
Medications
Several over-the-counter and prescription medications help manage GERD symptoms. Antacids provide quick relief from occasional heartburn. H2 blockers reduce acid production over several hours, while proton pump inhibitors offer longer-term acid suppression. Medication choice depends on symptom severity and frequency. Long-term treatment should be guided by a healthcare professional to prevent complications.
Medical Evaluation
Persistent or severe symptoms require medical evaluation. Diagnostic tests, such as endoscopy or pH monitoring, can confirm the presence of GERD and identify complications. In some cases, stronger medications or surgical interventions may be necessary to prevent further damage. Timely medical attention ensures both digestive and respiratory health are maintained.
When to Go to the ER?
Shortness of breath caused by GERD is usually mild, but certain warning signs require immediate medical attention. Seek urgent care if you notice any of the following:
- Severe difficulty breathing at rest: If you find it hard to breathe even while sitting or lying down, or feel like you can’t take a full breath, it may indicate a serious complication that requires immediate medical evaluation.
- Persistent chest pain or pressure: Continuous or worsening chest pain that does not improve with rest or usual remedies could signal a more serious condition, such as cardiac involvement or severe reflux-related complications.
- Bluish lips, face, or extreme fatigue: Any signs of low oxygen levels, including blue lips or fingertips, or sudden, overwhelming weakness, should be treated as an emergency.
- Continuous vomiting or severe nausea: Repeated vomiting can lead to dehydration, electrolyte imbalance, or esophageal injury. Prompt medical care is necessary to prevent further complications.
- Worsening cough or wheezing: A cough that intensifies despite home care, or new wheezing and respiratory distress, could indicate aspiration or worsening airway irritation.
- Difficulty swallowing or feeling of obstruction: If swallowing becomes painful or you feel food or liquid getting stuck in the throat, this could signal esophageal injury or obstruction, requiring immediate evaluation.
In any of these situations, visiting a facility like Neighbors Emergency Center ensures rapid assessment, proper diagnosis, and timely treatment to prevent serious complications.
Key Takeaways
- GERD can trigger shortness of breath, chest tightness, and asthma-like symptoms.
- Acid irritation, micro-aspiration, and vagus nerve reflexes are the main mechanisms.
- Lifestyle changes, medications, and medical evaluation help manage symptoms.
- Persistent or severe breathing difficulties may indicate serious complications.
- Immediate medical care, such as visiting an emergency room near me, is necessary for urgent symptoms.
FAQs
Q: What does GERD feel like?
GERD often feels like a burning sensation in the chest or throat, known as heartburn. It can also cause regurgitation, a sour taste, or discomfort when swallowing. Some people experience coughing or chest tightness along with these symptoms.
Q: How to avoid GERD?
Avoiding GERD involves lifestyle changes such as eating smaller meals, steering clear of trigger foods, and not lying down immediately after eating. Maintaining a healthy weight and reducing alcohol or smoking can also help prevent symptoms.
Q: Can GERD cause heart palpitations?
Yes, GERD can sometimes trigger heart palpitations due to acid irritating nerves near the esophagus. Stress and anxiety from discomfort may also contribute to a racing heartbeat. If palpitations are frequent or severe, medical evaluation is advised.
Summary
GERD can affect breathing through multiple mechanisms, including acid irritation, micro-aspiration, asthma-like responses, and vagus nerve reflexes. Symptoms such as shortness of breath, chest tightness, cough, and wheezing may accompany traditional reflux complaints. Lifestyle changes, medication, and medical evaluation are effective ways to manage both digestive and respiratory symptoms. Most cases are manageable, but persistent or severe shortness of breath should never be ignored. Seeking timely medical attention ensures long-term health and reduces the risk of complications.

